For UMN disease to cause palatal weakness it must be bilateral because there is bilateral UMN innervation for the nucleus ambiguus. corneal stimulation can also be performed by dropping a few drops of sterile saline onto the cornea from a height of 10 cm (less traumatic) reflex is present and intact if the patient blinks and eyes roll upwards. Patients with bilateral UMN weakness or dysfunction will lack voluntary movement of the palate but will have a hyperactive gag reflex (just like a hyperactive DTR with UMN disease). traditional method is to stroke the cornea with cotton wool. Gently touch first one and then the other palatal arch with a tongue blade, waiting each time for. Patients with bilateral LMN lesions have both absent voluntary and reflex activity. warn the patient that you are going to test the gag reflex. 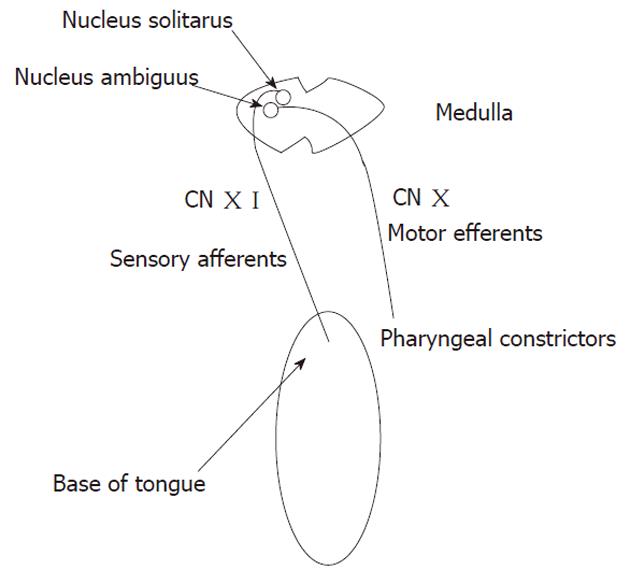
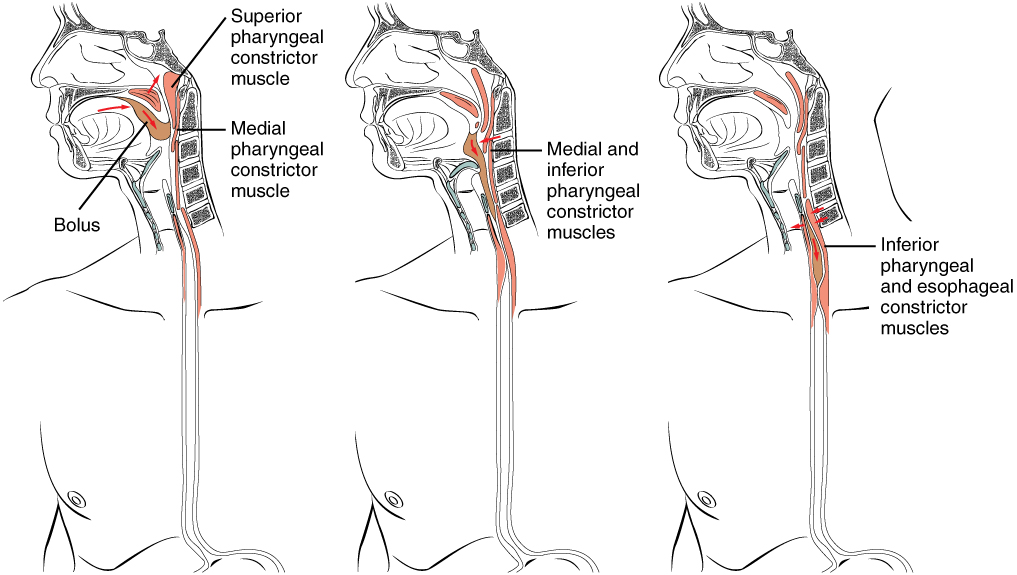
When a patient has weakness of the palatal muscles it is important to determine if this is from UMN vs. 
The patient has incomplete elevation of the palate with excessive nasal air escape when saying "pah" or "kah" (decreased volitional activity of CN 9 & 10) but a hyperactive gag reflex (increased non-voluntary or reflex motor action of CN 9 & 10). There are 12 of them, each named for its function or structure. The patient will have upper motor neuron signs including a positive jaw jerk and slow side-to-side tongue movements with the jaw frequently moving with the tongue. This cranial nerve examination OSCE guide provides a clear step-by-step approach to examining the cranial nerves, with an included video demonstration. Your cranial nerves are pairs of nerves that connect your brain to different parts of your head, neck, and trunk. The motor division of the glossopharyngeal nerve is derived. Glossopharyngeal nerve: Image of head structures including the glossopharyngeal nerve. 
It exits the brainstem out from the sides of the upper medulla, just rostral (closer to the nose) to the vagus nerve. If not, now you know a little more about this fascinating part of your oral cavity.Cranial Nerve Exam - Media Resources 01 - Pseudobulbar Palsy: Pseudobulbar palsy is caused by bilateral corticobulbar tract disease (UMN disease). The glossopharyngeal nerve is the ninth of 12 pairs of cranial nerves. If you are experiencing any numbness or pain in your mouth or throat and can't figure out why, talk to your dental professional or doctor to see if this may relate to your ninth cranial nerve. The glossopharyngeal nerve is amazing-it helps you taste, swallow, move muscles, produce saliva, and so much more, playing an essential role in your everyday life. In some cases, surgery can help take pressure off the nerve. Then, they will offer treatments such as anticonvulsant medications or local anesthesia. If your facial pain results from glossopharyngeal neuralgia, your medical professional may use MRI scans to assist with making a diagnosis. You may also be referred to a neurologist for further evaluation. Causes of Absent Pharyngeal Reflex Bulbar palsy - motor neuron disease, Guillain-Barr, polio, neurosyphilis, brainstem stroke Glossopharyngeal (IX) / vagus (. Your doctor will examine you for tumors, systemic conditions, and any history of injuries that could have affected your cranial nerves. They’ll likely ask you to explain your symptoms and perform a clinical exam on your head and neck to locate the source of the problem. If you think you’re experiencing glossopharyngeal nerve damage or issues, contact your doctor or dental professional. Because this nerve includes fibers with motor (movement) and sensory functions, doctors call it a “mixed nerve.” Cranial nerve (CN) testing is the physical functional assessment of the nerves arising from the brain and innervating the head, neck, and trunk. Finally, it helps move the throat during swallowing and talking, according to a review in the Journal of Neurosciences in Rural Practice. It also controls some motor fibers that help produce saliva as part of the parasympathetic nervous system, the system that's active when your body is resting and digesting. To help you visualize where this nerve is interacting with your oral cavity and throat, the University of Texas McGovern Medical School explains that this nerve is responsible for sensory fibers in the soft palate (roof of the mouth), the upper pharynx (throat), the tonsils, and the back portion of the tongue. Vagus nerve lesions produce palatal and pharyngeal. The glossopharyngeal nerve relays sensory information from many structures of the head and neck, provides taste sensations from the back of the tongue, helps with muscle contraction during swallowing, and stimulates saliva flow from the parotid glands. Glossopharyngeal nerve lesions produce difficulty swallowing impairment of taste over the posterior one-third of the tongue and palate impaired sensation over the posterior one-third of the tongue, palate, and pharynx an absent gag reflex and dysfunction of the parotid gland. The glossopharyngeal nerve stems out of the medulla oblongata, which is at the base of your brain and ends in the pharynx near the base of the tongue.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
